The Bio-Performance Protocol: The Complete System for Optimising Your Biological Hardware for Peak Cognitive and Physical Performance
Most people optimise one biological system and ignore the other four. Sleep without circadian anchoring drifts. Supplements without metabolic timing misfire. Exercise without recovery creates debt, not adaptation.
The systems nexus mapped alongside mapped below shows why integrated optimisation outperforms isolated interventions.
Five biological systems feed into one performance output — weakness in any one degrades them all.
Bio-performance is how well your body’s core biological systems work together to support peak output. Five systems drive it: sleep, hormones, cellular energy, nervous system regulation, and brain fuel. They don’t operate independently — poor sleep collapses hormone production, which drains energy, which weakens nervous system control. Optimising one without addressing the others creates a ceiling you can’t break through.
Sleep Architecture
The Two-Process Model governs every second of your recovery. Until you engineer both sleep pressure and circadian rhythm, every other system runs on compromised hardware.
Cognitive Fuel
Your brain burns through glucose and ketones on different metabolic highways. Time the wrong fuel source to the wrong task and you get brain fog, not focus.
Vagus Nerve Regulation
The vagus nerve carries 90% of body-to-brain signals. Low vagal tone doesn’t just mean poor recovery — it means your brain is operating on corrupted data.
Energy Systems
Mitochondria are the power plants of every cell you own. When they degrade, it’s not just fatigue — it’s a cap on every cognitive and physical process that runs on ATP.
Hormonal Optimisation
Testosterone, cortisol, thyroid, and growth hormone form a signalling cascade that governs recovery, drive, and resilience. One axis out of range and the entire system compensates.
TLDR: 10 Quick Wins. 10 Myths Busted.
10 tactics to deploy today + 10 myths holding you back — the 5-minute version of the full Bio-Performance protocol.
The Neuroscience of
Brain Health
Understanding the brain as a biological system. Complexity does not mean mystery; the brain operates according to measurable principles that can be optimized.
The Energy Imperative
Your brain is metabolically expensive. At rest, it consumes 20% of total body energy despite representing only 2% of body mass. During intense cognitive work, this scales to 25-30%.
- Continuous Fuel Dependence: Unlike muscle, the brain stores minimal energy (glycogen). It relies on constant delivery from the bloodstream.
- Vulnerability: High energy demand makes the brain exceptionally sensitive to glucose volatility and mitochondrial dysfunction.
- Substrate Flexibility: The brain can run on glucose (fed state) or ketones (fasted state). Flexibility is the marker of resilience.
The Neurotransmitter System
Neural communication relies on chemical messengers. Deficiency in precursors or cofactors impairs the entire network.
- Glutamate (Excitatory): Essential for learning. Excess leads to excitotoxicity.
- GABA (Inhibitory): The “brake pedal.” Balances excitation to prevent anxiety.
- Dopamine (Motivation): Drives executive function. Synthesized from Tyrosine.
- Serotonin (Mood): Regulates sleep-wake cycles. Synthesized from Tryptophan.
- Acetylcholine (Memory): Critical for attention. Synthesized from Choline.
Neuroplasticity: Adaptive Capacity
The brain reorganizes itself throughout life. Optimizing this process is the key to faster learning and recovery.
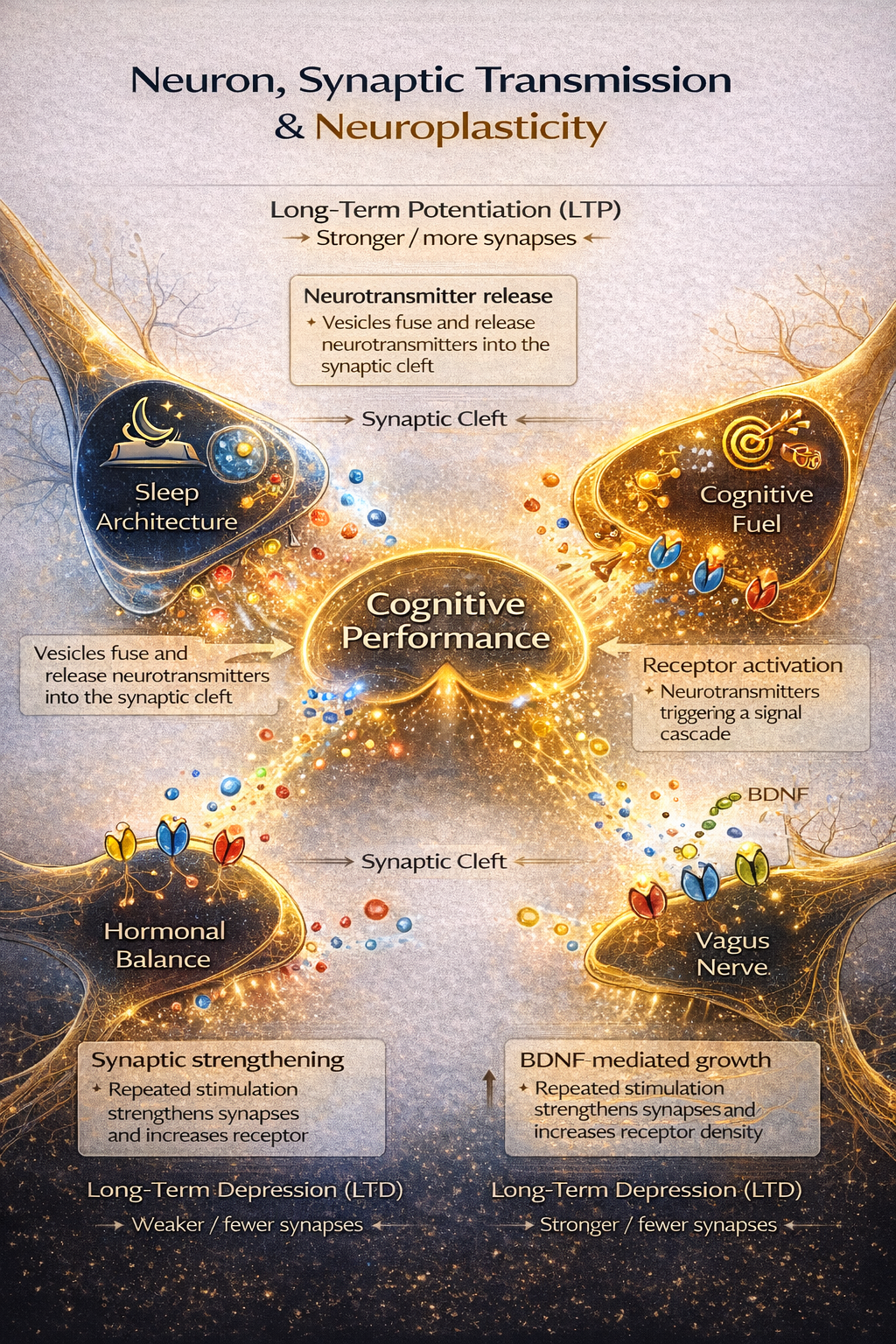
Structural Plasticity
Physical changes in dendritic spines and axonal branching. Occurs over days in response to learning.
Neurogenesis
Formation of new neurons in the hippocampus. Enhanced by BDNF, exercise, and Omega-3s.
The BDNF Factor: Brain-Derived Neurotrophic Factor is the master regulator. Exercise increases BDNF by 200-300%; sleep deprivation reduces it by 30-50%.
The Blood-Brain Barrier (BBB)
A highly selective membrane protecting the CNS. Its integrity determines neuroinflammation levels and cognitive clarity.
- Intact State: Excludes toxins and immune cells while transporting glucose and ketones.
- Compromised State: Inflammatory cytokines and neurotoxins enter, leading to “brain fog” and decline.
- Protection Protocol: Sleep consolidates tight junctions. Chronic cortisol increases permeability (“Leaky Brain”).
Brain fog isn’t one problem—it is a Multi-System Syndrome with various physiological failure modes.
The Five Pillars
In Depth
Pillar 1: Sleep Architecture
The Foundation of Neural Recovery
Sleep isn’t passive rest—it’s active biological maintenance during which critical processes occur that cannot happen during waking hours.
The Sleep Architecture Framework
Sleep cycles through distinct stages approximately every 90 minutes. Optimal sleep requires adequate time in all stages.
Critical Sleep-Dependent Processes
- Memory consolidation: Short-term memories transfer to long-term storage. SWS consolidates facts; REM consolidates skills. Learning followed by sleep improves retention by 20-40%.
- Synaptic homeostasis: Pruning weaker connections while preserving important ones to maintain neural efficiency and signal-to-noise ratio.
- Hormonal regulation: 70-80% of daily GH secretion occurs during deep sleep. Regulates cortisol, leptin, and ghrelin.
The Sleep Deprivation Cascade
Insufficient sleep (<7 hours) creates compound dysfunction:
Pillar 2: Cognitive Fuel
Metabolic Substrates for Function
Primary Fuel Sources
Metabolic Flexibility: The key isn’t dependence on one fuel, but the ability to utilize whichever substrate is available.
Neurotransmitter Precursors
Without precursors, synthesis fails regardless of health.
- Dopamine: Requires L-tyrosine + B6, iron, SAMe.
- Serotonin: Requires L-tryptophan + B6, magnesium.
- Acetylcholine: Requires choline + acetyl-CoA.
- GABA: Requires L-glutamate + B6, zinc.
Essential Structural Fats & Cofactors
Brain tissue is ~60% fat. Omega-3s (DHA) comprise 40% of phospholipids. Deficiency impairs membrane fluidity.
Micronutrients: B-vitamins (energy), Magnesium (ATP), Zinc (plasticity), Iron (oxygen), Selenium (antioxidant). Deficiency creates system-wide dysfunction.
Pillar 3: Vagus Nerve Regulation
The Stress Resilience Switch
The vagus nerve regulates heart rate, digestion, inflammation, and stress response—making it a master controller of physiological state.
Bidirectional Communication
80-90% of fibers are afferent (body-to-brain). Gut state and heart rhythm dictate mood. Top-down, mental state influences digestion.
Stimulation Techniques
- Controlled Breathing: Deep, slow breathing (4-6 breaths/min).
- Cold Exposure: Face in cold water or cold showers.
- Singing/Humming: Vocal cord vibration stimulates the nerve.
Pillar 4: Mitochondrial Energy
Cellular Power Production
Mitochondrial function directly determines cognitive capacity and resistance to mental fatigue. Neurons fire 5-50 times per second; each action potential costs ~100 million ATP.
Enhancing Function
- Exercise: HIIT creates the strongest signal for biogenesis (new mitochondria).
- Nutritional Support: CoQ10, PQQ, Magnesium, B-Vitamins.
- Hormetic Stress: Cold/heat exposure and fasting (autophagy) remove damaged organelles.
Pillar 5: Hormonal Optimization
Neurochemical Signaling
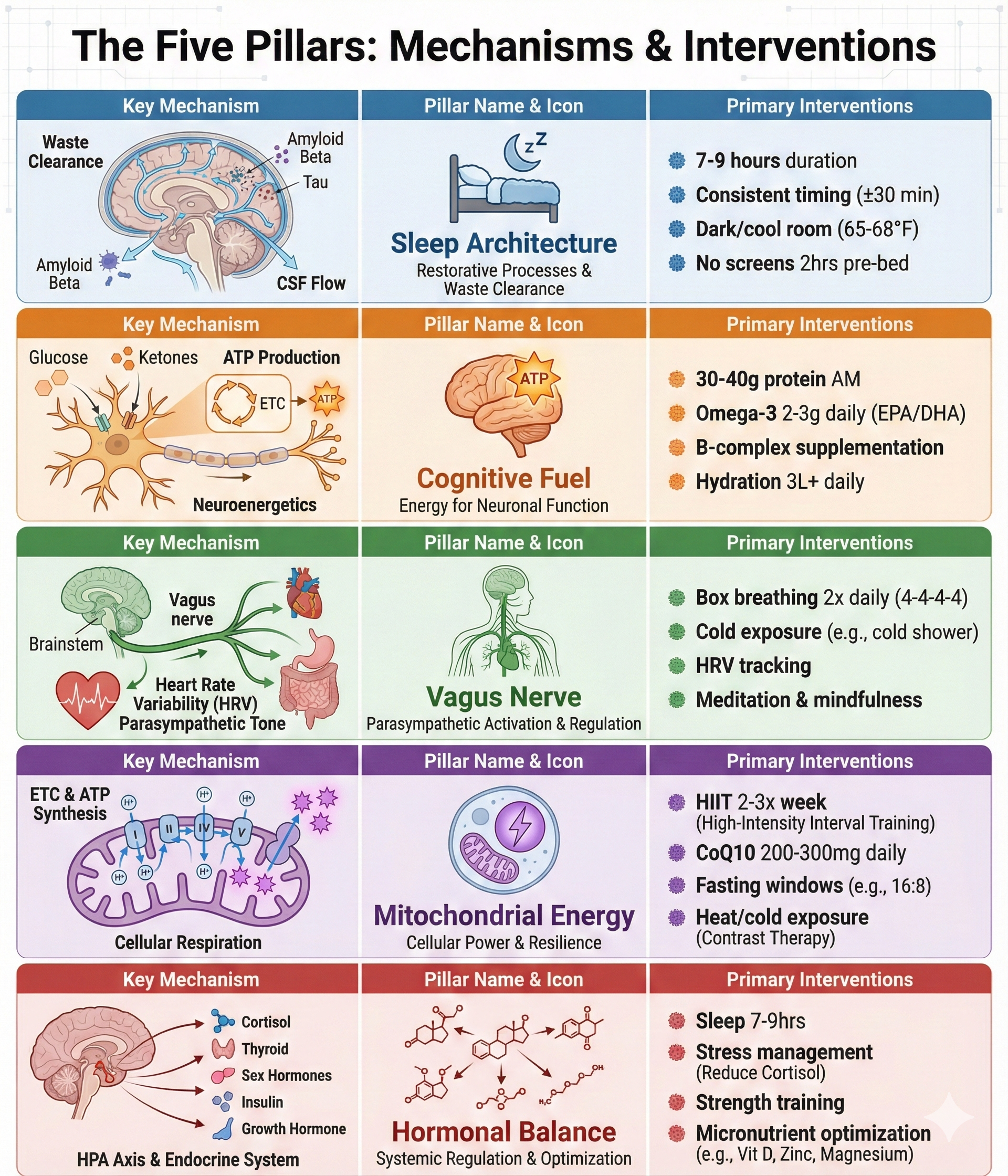
The five pillars aren’t separate interventions—they are interconnected systems.
The Science of
Integrated Optimization
The Synergistic Effect
Why Integration Outperforms Isolation
Optimizing single variables produces modest gains. Optimizing all five pillars simultaneously creates exponential improvements through synergistic interactions.
Research Evidence
- Combined Interventions: Studies show a 25% improvement in cognitive performance with combined protocols versus 8-12% for single interventions.
- Long-term Maintenance: Integrated protocols showed sustained benefits at 12-month follow-up, unlike isolated sleep optimization.
Biological Timing
Circadian Optimization
The brain operates on circadian rhythms—24-hour cycles governing virtually every physiological process. Aligning behaviors with circadian biology amplifies optimization effects.
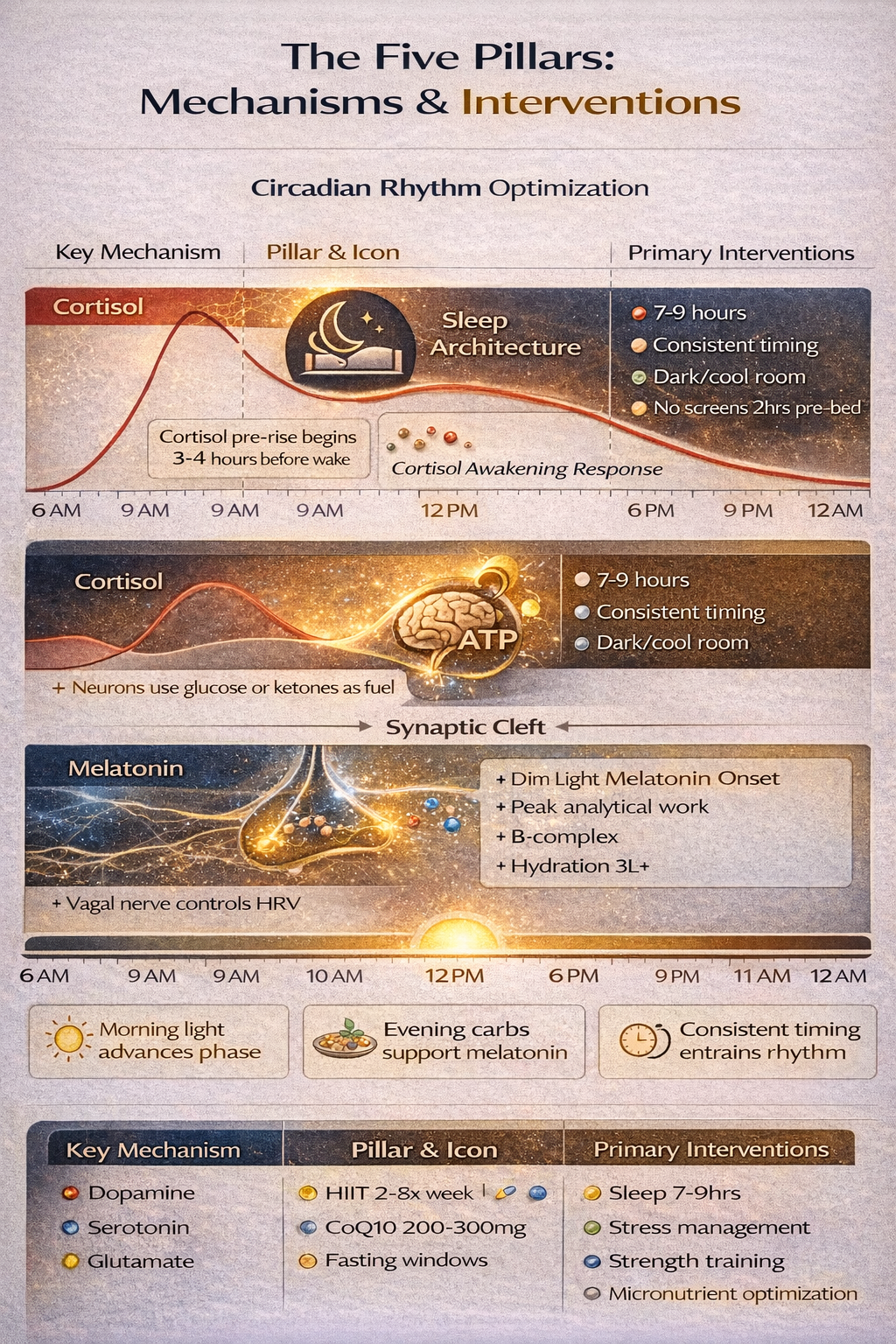
Optimization Strategies
Hormesis
Beneficial Stress for Adaptation
Hormesis describes beneficial adaptations from low-dose stressors that would be harmful at higher doses. The brain grows stronger through appropriate challenge.
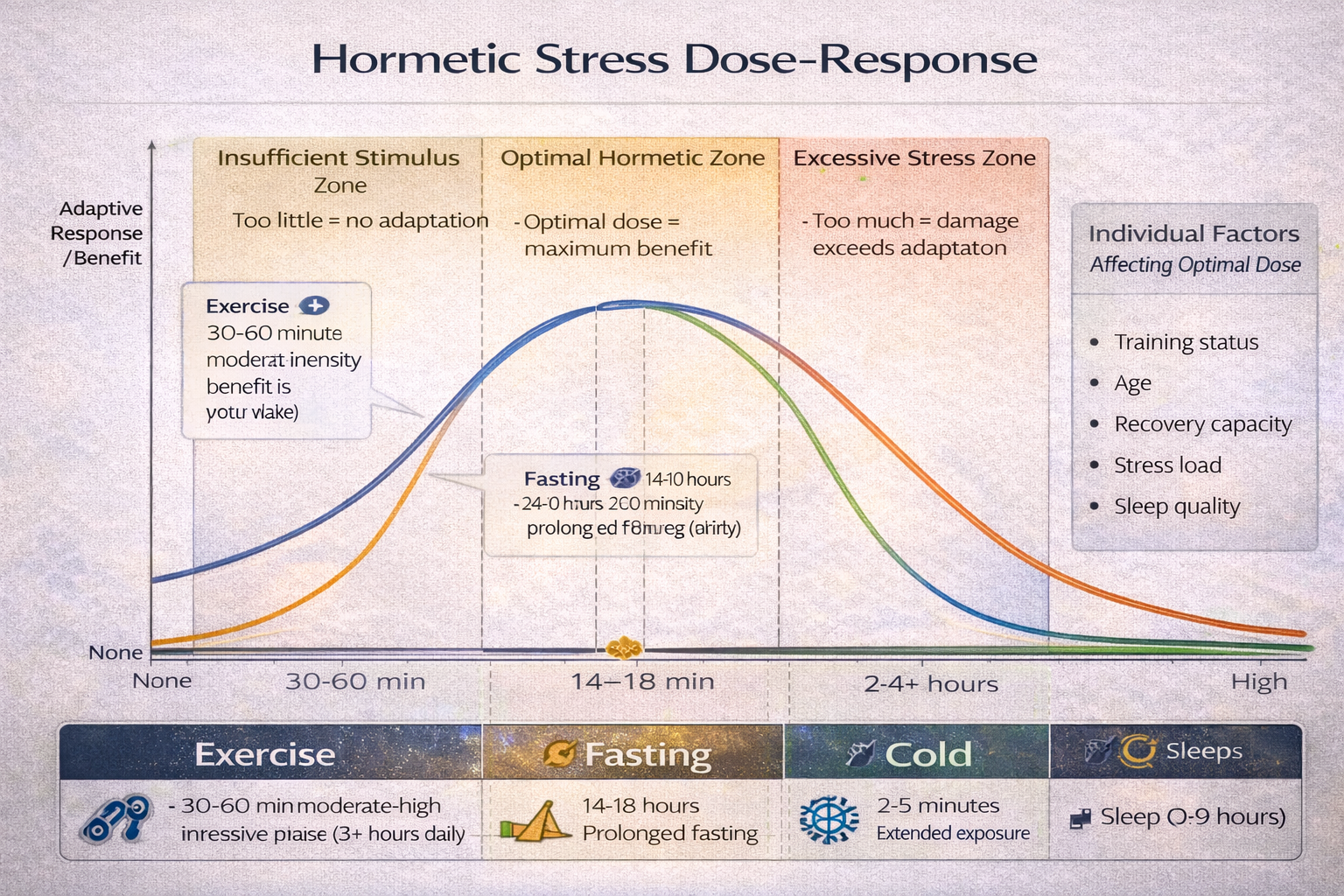
Hormetic Stressors for Brain Health
- Exercise: Creates transient oxidative stress, triggering BDNF release (up to 300%) and mitochondrial biogenesis.
- Fasting: Activates AMPK (energy sensor) and autophagy (cellular cleanup), enhancing neuroplasticity.
- Cold Exposure: Triggers norepinephrine release for focus and alertness; improves stress resilience.
- Heat Exposure (Sauna): Increases heat shock proteins (HSPs) which protect neurons and repair cellular damage.
Inflammation & Neuroprotection
Defense Systems
Chronic low-grade “neuroinflammation” contributes to cognitive decline, mood disorders, and impaired function. Reducing this load is essential for long-term health.
Brain optimization isn’t about doing more—it is about intelligent integration.
The Bio-Performance Protocol
A 90-day systematic programme to optimise your biology for peak cognitive performance — from sleep architecture and nutrition through neuroplasticity enhancement to permanent integration.
Based on Huberman, Ratey, Walker, and 40+ years of neuroscience and performance research
Day Complete
Great work on your bio-performance practice.
True elite performance is not sustained by brute force, but by metabolic flexibility and circadian precision.
Risks & Limitations
Risks, Limitations
& The Dark Side
Where biological optimisation fails — and the dangers of treating your body like a machine
Somewhere between the third supplement and the sixth biomarker, optimisation stops being a practice and starts being a religion. You feel sharper, sleep deeper, train harder — and the improvement itself becomes evidence that more will always mean better. It won't. Every protocol in this guide has failure modes, and the most insidious ones don't look like failure at all. They look like discipline. They look like commitment. They look like the kind of person who takes their health seriously — right up until the obsessive tracking, the rigid compliance, and the growing anxiety about missing a single metric reveal something closer to compulsion than performance.
Understanding where bio-performance protocols break down prevents overconfidence in your own compliance and reveals when professional medical guidance isn't just preferable — it's necessary. What follows is an honest accounting of the costs, the contraindications, and the people for whom aggressive biological optimisation does more harm than good.
Where Bio-Performance Optimisation Fails
These failure modes affect anyone who pursues biological optimisation. But for some, the risks are categorically different.
Who Should Not Use This Approach
Which of these describes you? Honest self-assessment is the first act of optimisation.
Critical Warning
The Dunning-Kruger Trap in Bio-Optimisation
Here is the cruellest irony of this entire guide: reading about biological optimisation makes you feel like an expert in your own biology. You learn about HPA axis regulation, mitochondrial biogenesis, and circadian gene expression — and you start believing you can self-diagnose, self-prescribe, and self-treat. This is the Dunning-Kruger effect applied to health: a little knowledge creates dangerous overconfidence. You are not a doctor, an endocrinologist, or a sleep specialist — no matter how many peer-reviewed papers you've read.
Self-Assessment — Check Any That Apply
- You adjust supplement dosages based on how you "feel" rather than blood work
- You dismiss your doctor's advice because "they don't understand performance optimisation"
- You diagnose your own hormonal issues based on symptoms and internet research
- You've been optimising for 6+ months without a single blood panel or medical consultation
Protection Against Overconfidence
- Get baseline blood work before starting and retest every 3–6 months — objective data prevents false confidence
- Maintain a relationship with a physician who understands performance contexts — not Dr. Google
- Default assumption: "My biology may respond differently" rather than "This will definitely work for me"
- Track objective biomarkers (HRV, sleep architecture, blood panels) — subjective "feeling good" is unreliable
Failure modes and exclusions describe individual risks. But the deepest limitations aren't personal — they're environmental and structural. This is the Bio-Performance Protocol.
The Limits of Individual Bio-Optimisation
Most consequential health outcomes are determined by factors beyond individual protocol compliance. Optimising your biology in an environment that undermines it is like tuning an engine while driving on roads full of potholes.
If you have the resources and influence to address these structural constraints, these interventions compound the value of individual optimisation.
Environment-Level Solutions
- Negotiate work boundaries that protect sleep and recovery — the research on cognitive performance and sleep makes the business case irrefutable
- Invest in air and water filtration — HEPA filters and reverse osmosis systems remove environmental pollutants that no supplement can neutralise
- Build a medical team rather than relying on a single GP — a sports medicine physician, a functional medicine practitioner, and your primary care doctor covering different domains
- Create peer accountability through training partners or mastermind groups — social support is itself a powerful health intervention with independent effects on cortisol and immune function
- Advocate for workplace wellness policies — standing desks, natural light, meeting-free focus blocks, and flexible schedules benefit entire organisations, not just individuals
The goal was never perfection. It was better biology, compounding daily — with the humility to know what medicine can do that willpower cannot.
The risks of bio-optimisation are real: obsessive tracking, supplement dependency, recovery deficits, and above all, the Dunning-Kruger trap that makes you overconfident in your own biological expertise. Respect these failure modes — your biology is more complex than any protocol.
Your Questions Answered
16 research-backed answers covering the science, practice, and application of bio-performance — from brain health fundamentals to building your optimization protocol.
No questions match your search
Try different keywords or
01What exactly is the Bio-Performance Protocol?
The Bio-Performance Protocol is a systematic, evidence-based framework for optimising cognitive function across five interconnected biological systems — sleep, nutrition, nervous system regulation, mitochondrial energy, and hormonal balance.
Unlike isolated "brain hacks," the protocol treats your brain as a metabolically expensive organ that consumes 20% of total body energy despite being just 2% of body mass. Performance depends on the integrity of all five systems working together. A deficiency in any single pillar — poor sleep, unstable blood sugar, chronic stress, mitochondrial dysfunction, or hormonal imbalance — creates cascading effects across the entire network. The protocol addresses all five simultaneously because integrated interventions produce 25% cognitive improvement versus 8–12% from single-variable approaches.
A financial analyst sleeping 6 hours, skipping breakfast, and relying on caffeine might score normally on an IQ test but lose 30–40% of their decision-making capacity by 2pm. The protocol doesn't add a supplement — it restructures sleep timing, meal composition, caffeine strategy, and stress management as one coordinated system.
It's biological systems engineering for your brain — not a supplement stack, not a single habit, but a coordinated optimisation of the five systems that determine whether you experience brain fog or high-velocity clarity. **Citations:** 1. Raichle, M. E. & Gusnard, D. A. (2002). Appraising the brain's energy budget. *PNAS*, 99(16), 10237–10239. 2. Ngandu, T. et al. (2015). A 2 year multidomain intervention of diet, exercise, cognitive training, and vascular risk monitoring versus control to prevent cognitive decline. *The Lancet*, 385(9984), 2255–2263.
02Why does the brain consume so much energy?
Your brain fires 5–50 electrical impulses per second across 86 billion neurons — each action potential costs roughly 100 million ATP molecules — making it the most metabolically demanding organ in your body.
At rest, the brain uses 20% of total body energy. During intense cognitive work, this scales to 25–30%. Unlike muscle, the brain stores virtually no energy reserves (minimal glycogen), meaning it depends on continuous delivery from the bloodstream. This creates a critical vulnerability: even brief disruptions in glucose stability, oxygen delivery, or mitochondrial function produce immediate cognitive impairment. The brain can run on glucose (fed state) or ketones (fasted state), and metabolic flexibility between these fuels is itself a marker of cognitive resilience.
After a high-sugar lunch, blood glucose spikes then crashes within 90 minutes. During the crash, your prefrontal cortex — responsible for executive function and decision-making — is essentially running on fumes. That 3pm "brain fog" isn't laziness; it's a measurable fuel delivery failure.
The brain's extraordinary energy demand is both its superpower and its weakness. Feed it precisely and it performs at levels most people never experience. Starve it — even slightly — and cognitive capacity drops immediately. **Citations:** 1. Attwell, D. & Laughlin, S. B. (2001). An energy budget for signaling in the grey matter of the brain. *Journal of Cerebral Blood Flow & Metabolism*, 21(10), 1133–1145. 2. Mergenthaler, P. et al. (2013). Sugar for the brain: the role of glucose in physiological and pathological brain function. *Trends in Neurosciences*, 36(10), 587–597.
03What causes brain fog and how do I fix it?
Brain fog isn't a single problem — it's a multi-system syndrome with at least six distinct physiological failure modes, each requiring a different intervention.
The six pathways to brain fog are: glucose dysregulation (blood sugar volatility), neurotransmitter precursor deficiency (missing building blocks for dopamine, serotonin, acetylcholine), gut-brain dysfunction (compromised vagal signaling), mitochondrial impairment (cellular energy production failure), neuroinflammation (blood-brain barrier compromise), and sleep architecture disruption (inadequate glymphatic clearance). Most people address only one — typically caffeine to mask adenosine — while the underlying causes compound. Effective protocols address all pathways simultaneously because solving for only one variable leaves the syndrome intact.
A startup founder experiencing persistent afternoon fog might assume they need more coffee. But testing reveals their fog stems from three simultaneous failures: a high-carb lunch crashing glucose, chronic stress elevating cortisol (impairing hippocampal function), and 5.5 hours of fragmented sleep preventing glymphatic waste clearance. Caffeine masks the adenosine signal while all three root causes worsen.
Identify which of the six pathways is driving your fog. The protocol's diagnostic approach tests each systematically rather than applying generic fixes. **Citations:** 1. Ocon, A. J. (2013). Caught in the thickness of brain fog: exploring the cognitive symptoms of chronic fatigue syndrome. *Frontiers in Physiology*, 4, 63. 2. Xie, L. et al. (2013). Sleep drives metabolite clearance from the adult brain. *Science*, 342(6156), 373–377.
04What is neuroplasticity and can I actually improve it?
Neuroplasticity is your brain's ability to physically reorganise itself — forming new neural connections, strengthening existing ones, and even generating new neurons — and yes, you can dramatically enhance it at any age.
Structural plasticity involves physical changes in dendritic spines and axonal branching, occurring over days in response to learning. Neurogenesis — the formation of entirely new neurons — occurs throughout life in the hippocampus. The master regulator of both processes is Brain-Derived Neurotrophic Factor (BDNF). Exercise increases BDNF by 200–300%, while sleep deprivation reduces it by 30–50%. Omega-3 fatty acids (particularly DHA) support the membrane structure of new neurons, and novel skill learning — languages, musical instruments — provides broader cognitive benefits than any brain training game.
London taxi drivers who spend years memorising 25,000 streets show measurably larger hippocampi than bus drivers who follow fixed routes. The brain physically expanded in response to sustained cognitive demand — and this capacity doesn't diminish with age, only with disuse.
Your brain is constantly remodelling itself. The question isn't whether neuroplasticity exists — it's whether you're directing it intentionally through exercise, sleep, nutrition, and novel learning, or letting it atrophy by default. **Citations:** 1. Maguire, E. A. et al. (2000). Navigation-related structural change in the hippocampi of taxi drivers. *PNAS*, 97(8), 4398–4403. 2. Cotman, C. W. & Berchtold, N. C. (2002). Exercise: a behavioral intervention to enhance brain health and plasticity. *Trends in Neurosciences*, 25(6), 295–301.
05What is the blood-brain barrier and why should I care?
The blood-brain barrier is a highly selective membrane that protects your central nervous system from toxins and pathogens — and when it's compromised by chronic stress, poor sleep, or inflammation, the result is persistent brain fog and accelerated cognitive decline.
In its intact state, the BBB excludes harmful molecules and immune cells while selectively transporting glucose, ketones, and essential nutrients into brain tissue. Chronic cortisol elevation, sleep deprivation, gut dysbiosis, and systemic inflammation all increase BBB permeability — sometimes called "leaky brain." When the barrier becomes permeable, inflammatory cytokines and neurotoxins enter brain tissue, triggering neuroinflammation. Sleep consolidates the tight junctions that maintain barrier integrity, which is one reason why chronic sleep deprivation produces cognitive symptoms that no amount of caffeine can resolve.
Researchers studying shift workers found that those working rotating night shifts for more than 10 years showed BBB permeability markers equivalent to early-stage neuroinflammation, along with measurable declines in processing speed and working memory that persisted even after returning to normal schedules.
Protecting your blood-brain barrier through sleep quality, stress management, and anti-inflammatory nutrition is foundational — without it, every other optimisation you attempt reaches your brain through a compromised filter. **Citations:** 1. Montagne, A. et al. (2015). Blood-brain barrier breakdown in the aging human hippocampus. *Neuron*, 85(2), 296–302. 2. Hurtado-Alvarado, G. et al. (2016). Blood-brain barrier disruption induced by chronic sleep loss. *International Journal of Molecular Sciences*, 18(11), 2431.
06Is cognitive decline actually inevitable with age?
No. Age-related cognitive decline is largely modifiable through lifestyle factors — individuals maintaining optimal sleep, nutrition, and exercise preserve function equivalent to people 10–20 years younger.
Biological age and chronological age are not the same thing. The FINGER trial — a landmark 2-year randomised controlled study — demonstrated that a multi-domain intervention (diet, exercise, cognitive training, and vascular risk management) significantly improved or maintained cognitive function in at-risk older adults compared to controls receiving standard health advice. The brain retains neuroplasticity throughout life; neurogenesis continues in the hippocampus into old age. What accelerates decline isn't aging itself but the cumulative damage from chronic inflammation, sleep deprivation, metabolic dysfunction, and physical inactivity — all of which are addressable.
A 70-year-old marathon runner who sleeps 7–8 hours, follows a Mediterranean diet, and learns new skills regularly can outperform a sedentary 45-year-old on working memory and processing speed tests. The difference isn't genetics — it's decades of compounding biological optimisation versus decades of compounding biological neglect.
Cognitive decline is not a sentence — it's a trajectory you can change at any point. The protocol works at every age; starting earlier simply means more years of compounding benefit. **Citations:** 1. Ngandu, T. et al. (2015). A 2 year multidomain intervention of diet, exercise, cognitive training, and vascular risk monitoring versus control to prevent cognitive decline in at-risk elderly people (FINGER). *The Lancet*, 385(9984), 2255–2263. 2. Erickson, K. I. et al. (2011). Exercise training increases size of hippocampus and improves memory. *PNAS*, 108(7), 3017–3022.
07What should I eat for optimal brain performance?
Your brain needs three categories of fuel delivered in the right sequence: stable glucose or ketones for energy, amino acid precursors for neurotransmitter synthesis, and structural fats (especially DHA) for membrane integrity.
The brain consumes approximately 120g of glucose per day in a fed state, but it can also run on ketones during fasting, which produce energy more efficiently with fewer reactive oxygen species. The critical neurotransmitter precursors are: L-tyrosine (for dopamine), L-tryptophan (for serotonin), and choline (for acetylcholine). Without these building blocks, synthesis fails regardless of how healthy you are otherwise. Brain tissue is approximately 60% fat by dry weight, with DHA (an omega-3 fatty acid) comprising 40% of neuronal phospholipids. Deficiency impairs membrane fluidity and signal transmission. The essential cofactors — B-vitamins, magnesium, zinc, iron, selenium — act as catalysts across all these processes.
A high-protein breakfast (30–40g within 90 minutes of waking) provides tyrosine for dopamine production when synthesis capacity is at its peak. Combining this with omega-3 rich foods (wild salmon, sardines) or 2–3g EPA/DHA supplementation supports the structural integrity of the neurons doing the work.
Think of nutrition as brain engineering: glucose/ketones for power, amino acids for communication, omega-3s for structure, and micronutrients as the catalysts that make everything run. Miss any category and the system degrades. **Citations:** 1. Gómez-Pinilla, F. (2008). Brain foods: the effects of nutrients on brain function. *Nature Reviews Neuroscience*, 9(7), 568–578. 2. Bourre, J. M. (2006). Effects of nutrients (in food) on the structure and function of the nervous system. *Journal of Nutrition, Health & Aging*, 10(5), 377–385.
08How does caffeine actually work, and am I using it wrong?
Caffeine doesn't give you energy — it blocks the adenosine receptors that signal tiredness, masking fatigue without addressing the underlying metabolic debt that caused it.
Adenosine is a byproduct of neural activity that accumulates throughout the day, binding to receptors that promote sleepiness. Caffeine's molecular structure is similar enough to adenosine that it occupies the same receptors without activating them — essentially jamming the "tired" signal. The problem: adenosine continues building up behind the blockade. When caffeine wears off, all that accumulated adenosine floods your receptors simultaneously, creating the afternoon crash. Strategic caffeine timing means delaying first intake 90–120 minutes post-waking (allowing your natural cortisol awakening response to clear adenosine naturally) and stopping by early afternoon to prevent sleep architecture disruption.
Most people drink coffee immediately upon waking, when cortisol is already at its peak. This wastes caffeine's effect (you're already alert), builds tolerance faster, and creates dependency. Delaying to 9:30–10am for a 7:30am waker aligns caffeine with the natural cortisol dip, producing stronger focus without the crash.
Caffeine is a precision tool, not a crutch. Time it strategically, stop by early afternoon, and never use it to compensate for sleep debt — it masks the signal but worsens the underlying problem. **Citations:** 1. Reichert, C. F. et al. (2022). Caffeine, adenosine receptors, and sleep. *Handbook of Experimental Pharmacology*, 253, 101–133. 2. Drake, C. et al. (2013). Caffeine effects on sleep taken 0, 3, or 6 hours before going to bed. *Journal of Clinical Sleep Medicine*, 9(11), 1195–1200.
09Do nootropics and supplements actually work?
Supplements amplify an optimised baseline — no nootropic stack can compensate for chronic sleep debt, poor nutrition, or sedentary behaviour, but targeted compounds provide genuine marginal gains on top of solid foundations.
Exercise increases BDNF 3x more than any supplement. That's the honest starting point. However, once the foundational pillars are solid, certain compounds have robust evidence: omega-3s (2–3g EPA/DHA) for membrane integrity and anti-inflammation, creatine (3–5g) for ATP buffering in the brain, magnesium (particularly glycinate or threonate) for synaptic function and sleep quality, and vitamin D for neuroprotection if deficient. The nootropics with strongest evidence include lion's mane mushroom (for nerve growth factor stimulation) and phosphatidylserine (for cortisol modulation). Most marketed "brain supplements" have minimal evidence and rely on proprietary blends that obscure dosing.
A software engineer optimising sleep (7.5 hours), eating adequate protein, exercising 4x/week, and managing stress adds creatine and omega-3s. They notice a measurable improvement in afternoon focus and working memory. Their colleague, sleeping 5 hours and eating poorly, takes the same supplements and notices nothing — the deficit is too large for supplements to bridge.
Build the metabolic base first through sleep, nutrition, exercise, and stress management. Then layer targeted, evidence-backed supplements for the final 5–10% of optimisation. Skip the hype stacks. **Citations:** 1. Avgerinos, K. I. et al. (2018). Effects of creatine supplementation on cognitive function of healthy individuals. *Experimental Gerontology*, 108, 166–173. 2. Mori, K. et al. (2009). Improving effects of the mushroom *Yamabushitake* (Hericium erinaceus) on mild cognitive impairment. *Phytotherapy Research*, 23(3), 367–372.
10What's the deal with glucose versus ketones for brain fuel?
Your brain can run on two fuel sources — glucose (default, fed state) and ketones (fasting or ketogenic state) — and the ability to switch between them, called metabolic flexibility, is itself a powerful marker of cognitive resilience.
In a standard fed state, the brain consumes approximately 120g of glucose daily, transported across the blood-brain barrier via GLUT1 and GLUT3 transporters. Glucose produces 30–36 ATP molecules per unit via oxidative phosphorylation. Ketones (primarily beta-hydroxybutyrate) produce slightly fewer ATP (~27) but with higher thermodynamic efficiency and significantly fewer reactive oxygen species — meaning cleaner energy with less oxidative damage. During prolonged fasting or ketosis, ketones can supply up to 70% of the brain's energy needs. The performance advantage isn't about choosing one fuel permanently — it's about training your metabolism to use whichever is available, preventing the cognitive collapse that occurs when glucose-dependent brains experience even mild hypoglycaemia.
An executive who practises intermittent fasting (16:8 window) develops metabolic flexibility over 4–6 weeks. During a 12-hour negotiation day where meals are unpredictable, their brain seamlessly shifts to ketone metabolism while their glucose-dependent colleague experiences progressive cognitive degradation after missing lunch.
Train metabolic flexibility through occasional fasting, not permanent ketosis. The goal is a brain that performs on any fuel available — glucose abundance or scarcity. **Citations:** 1. Cunnane, S. C. et al. (2016). Can ketones compensate for deteriorating brain glucose uptake during aging? *Annals of the New York Academy of Sciences*, 1367(1), 12–20. 2. Cahill, G. F. (2006). Fuel metabolism in starvation. *Annual Review of Nutrition*, 26, 1–22.
11Why is sleep the single most important performance variable?
During deep sleep, your brain activates its glymphatic waste clearance system — expanding interstitial space by 60% to flush neurotoxic proteins like beta-amyloid and tau — a process that cannot occur during waking hours at any meaningful level.
Sleep isn't passive rest; it's active biological maintenance. Memory consolidation transfers short-term memories to long-term storage (SWS consolidates facts, REM consolidates skills). Synaptic homeostasis prunes weaker connections while preserving important ones. 70–80% of daily growth hormone secretion occurs during deep sleep. After just 24 hours without sleep, cognitive performance equals a blood alcohol level of 0.1% — legally drunk. Chronic restriction below 7 hours creates compound dysfunction: insulin sensitivity drops 30–40%, natural killer cell activity falls 70%, and amygdala reactivity increases 60%, making you simultaneously less intelligent, less healthy, and more emotionally reactive.
A surgeon sleeping 6 hours nightly may feel "fine" but objective testing shows their procedural accuracy drops 20% and their reaction time matches someone with significant alcohol impairment. The insidious part of sleep deprivation is that self-assessment of impairment is the first faculty to degrade — you feel fine precisely because you've lost the capacity to notice you're not.
Sleep is the foundation that every other optimisation depends on. No supplement, diet, or training protocol can compensate for inadequate sleep. Fix this first; everything else compounds on top of it. **Citations:** 1. Xie, L. et al. (2013). Sleep drives metabolite clearance from the adult brain. *Science*, 342(6156), 373–377. 2. Lim, J. & Dinges, D. F. (2010). A meta-analysis of the impact of short-term sleep deprivation on cognitive variables. *Psychological Bulletin*, 136(3), 375–389.
12What is the vagus nerve and how does it affect my performance?
The vagus nerve is the longest cranial nerve in your body, connecting brain to gut, heart, and lungs — and its "tone" (responsiveness) is the primary biomarker that distinguishes stress-resilient high performers from those who crumble under pressure.
High vagal tone correlates with better emotional regulation, enhanced cognition under stress, reduced systemic inflammation, and faster recovery between high-demand periods. Low vagal tone correlates with chronic anxiety, impaired recovery, elevated inflammation, and persistent brain fog. Critically, 80–90% of vagal fibres are afferent (body-to-brain), meaning your gut state and heart rhythm directly dictate your mood and cognitive capacity — not the other way around. Stimulation techniques include controlled deep breathing (4–6 breaths per minute), cold exposure (face immersion or cold showers), singing or humming (vocal cord vibration activates the nerve), and heart rate variability (HRV) training.
An elite military operator practises box breathing (4-count inhale/hold/exhale/hold) for 5 minutes before a high-stakes briefing. Their HRV data shows parasympathetic activation within 90 seconds, measurably reducing cortisol and improving prefrontal function — the opposite of the "freeze" response their untrained colleagues experience.
Your vagus nerve is the master switch between fight-or-flight reactivity and calm, focused performance. Training it through breathing, cold exposure, and HRV biofeedback is one of the highest-ROI investments in cognitive performance. **Citations:** 1. Breit, S. et al. (2018). Vagus nerve as modulator of the brain-gut axis in psychiatric and inflammatory disorders. *Frontiers in Psychiatry*, 9, 44. 2. Laborde, S. et al. (2017). Heart rate variability and cardiac vagal tone in psychophysiological research. *Frontiers in Psychology*, 8, 213.
13What is hormesis and why should I deliberately stress my body?
Hormesis is the biological principle that low-dose stressors — exercise, cold exposure, fasting, heat — trigger adaptive responses that make your brain and body stronger, as long as you allow adequate recovery between exposures.
The dose-response curve is key: too little stress produces no adaptation, the right amount triggers growth, and too much causes damage. Exercise creates transient oxidative stress that triggers BDNF release (up to 300%) and mitochondrial biogenesis (new mitochondria). Fasting activates AMPK (the cellular energy sensor) and autophagy (cellular cleanup), enhancing neuroplasticity. Cold exposure triggers norepinephrine release for immediate alertness and long-term stress resilience. Heat exposure (sauna) increases heat shock proteins that protect neural tissue. The critical variable is recovery — without adequate sleep, nutrition, and rest between hormetic stressors, you shift from adaptation to accumulated damage.
A 30-second cold shower ending isn't torture — it's a precise norepinephrine trigger. Studies show cold exposure increases norepinephrine by 200–300%, producing hours of enhanced alertness and focus. But doing this after a night of 4 hours sleep adds stress to an already depleted system — hormesis requires a foundation of recovery to work.
Controlled, deliberate stress followed by adequate recovery is how biological systems upgrade. The protocol uses exercise, cold, fasting, and heat as precision tools — not punishments. **Citations:** 1. Mattson, M. P. (2008). Hormesis defined. *Ageing Research Reviews*, 7(1), 1–7. 2. Šrámek, P. et al. (2000). Human physiological responses to immersion into water of different temperatures. *European Journal of Applied Physiology*, 81(5), 436–442.
14How does chronic stress physically damage my brain?
Chronic stress isn't psychological — it's structural. Sustained cortisol elevation causes measurable hippocampal shrinkage, amygdala enlargement, and prefrontal cortex thinning, physically degrading the brain regions responsible for memory, emotional regulation, and executive function.
Elevated cortisol directly kills hippocampal neurons, reduces neurogenesis, and damages synaptic connections — shrinking the brain structure most critical for learning and memory. Simultaneously, the amygdala (threat detection centre) grows larger and more reactive, creating a hypervigilant state that impairs rational thinking. The prefrontal cortex — seat of planning, decision-making, and impulse control — thins under chronic stress, reducing executive function precisely when you need it most. Additionally, chronic cortisol increases blood-brain barrier permeability, allowing inflammatory molecules to enter brain tissue and sustaining a neuroinflammatory cycle.
MRI studies of corporate executives working 80+ hour weeks for 3+ years show hippocampal volumes 10–15% below age-matched controls, with corresponding impairments in episodic memory and cognitive flexibility. The cruel irony: the people working hardest to succeed are physically degrading the brain regions that make success possible.
Stress management isn't soft — it's structural brain protection. Every hour invested in recovery protocols (sleep, breathing, exercise) directly preserves the neural architecture that produces your best work. **Citations:** 1. McEwen, B. S. (2007). Physiology and neurobiology of stress and adaptation: central role of the brain. *Physiological Reviews*, 87(3), 873–904. 2. Lupien, S. J. et al. (2009). Effects of stress throughout the lifespan on the brain, behaviour and cognition. *Nature Reviews Neuroscience*, 10(6), 434–445.
15Where should I start if I'm completely new to bio-optimisation?
Start with sleep. Fix your sleep architecture first — every other optimisation in the protocol produces dramatically better results when built on a foundation of 7–8 hours of quality sleep.
The recommended entry sequence is: (1) Sleep — establish a consistent 7–8 hour window with the bedroom screen-free, cool (18°C), and dark. This alone resolves a significant portion of brain fog within 7–14 days. (2) Morning routine — sunlight within 60 minutes of waking, 500–750ml water, delay caffeine 90 minutes. (3) Nutrition basics — 30–40g protein at breakfast, reduce refined sugar, add omega-3 supplementation. (4) Movement — insert 2–3 minute movement breaks every 90 minutes during cognitive work. (5) Stress — 5 minutes of box breathing twice daily. Don't try to implement everything simultaneously. The protocol is designed for progressive layering over 30 days.
Week 1: fix sleep timing and screen removal. Week 2: add morning sunlight and delayed caffeine. Week 3: optimise breakfast protein and begin omega-3s. Week 4: add box breathing and movement snacking. Each layer builds on the last, and the progressive approach prevents the overwhelm that causes most optimisation attempts to fail within 72 hours.
Sleep first, then morning routine, then nutrition, then movement, then stress management. Progressive layering over 30 days. Don't try to change everything at once. **Citations:** 1. Walker, M. (2017). *Why We Sleep: Unlocking the Power of Sleep and Dreams*. Scribner. 2. Lally, P. et al. (2010). How are habits formed: Modelling habit formation in the real world. *European Journal of Social Psychology*, 40(6), 998–1009.
16What results can I realistically expect, and how quickly?
Most people notice reduced brain fog and improved morning clarity within 7–14 days of fixing sleep and hydration. Measurable improvements in sustained focus, emotional regulation, and cognitive endurance typically emerge by week 3–4 of the full protocol.
The timeline depends on which systems are most compromised. Sleep improvements produce the fastest results because glymphatic clearance begins improving on the first night of adequate sleep. Nutritional changes take 2–3 weeks as neurotransmitter precursor levels stabilise and membrane composition shifts. Vagal tone improvements from daily breathing practice show measurable HRV changes within 2–4 weeks. Exercise-driven BDNF increases are detectable within days but functional neuroplasticity benefits compound over months. The full integrated protocol produces its strongest results at the 8–12 week mark, when all five systems have reached a new equilibrium. Realistic expectations: 20–30% improvement in sustained attention, significant reduction in afternoon cognitive crashes, better stress recovery, and improved sleep quality metrics.
A 42-year-old marketing director implemented the protocol progressively over 30 days. By day 10, morning brain fog had resolved. By week 3, she reported sustained focus through 3pm without caffeine (previously needed 3 cups by noon). At week 8, her HRV had increased 15% and she described the change as "having a brain that actually works all day instead of just in the morning."
Expect early wins in 1–2 weeks (fog reduction, morning clarity), meaningful performance shifts at 3–4 weeks, and full system optimisation at 8–12 weeks. The compound effects continue indefinitely. **Citations:** 1. Ngandu, T. et al. (2015). A 2 year multidomain intervention of diet, exercise, cognitive training, and vascular risk monitoring. *The Lancet*, 385(9984), 2255–2263. 2. Cotman, C. W. et al. (2007). Exercise builds brain health: key roles of growth factor cascades and inflammation. *Trends in Neurosciences*, 30(9), 464–472.
You've explored all 16 questions
Ready to go deeper? The full Bio-Performance Protocol article provides comprehensive frameworks, implementation protocols, and advanced optimization systems.
Engineering Your Biological Foundation
Cognitive performance isn't a software problem—it's a hardware problem. You can't willpower your way through metabolic dysfunction, sleep deprivation, or autonomic dysregulation. The brain is a biological organ with specific requirements for optimal function. Meet those requirements systematically, and performance emerges naturally.
The Protocol Framework
- Tier 1 (Foundation): Circadian optimization, sleep architecture, metabolic flexibility, autonomic regulation, hormonal balance. These aren't optional enhancements—they're prerequisites. Master these first.
- Tier 2 (Enhancement): Strategic supplementation, advanced metabolic protocols, cognitive training, recovery optimization. Build on foundation once established.
- Tier 3 (Precision): Individual response data, biomarker tracking, personalized optimization. Refine based on YOUR biology, not population averages.
The 80/20 Principle
80% of benefits come from foundational protocols—sleep, light exposure, protein-first nutrition, omega-3 supplementation, stress management. These are high-leverage, low-risk interventions anyone can implement immediately. The remaining 20% comes from advanced optimization requiring more complexity, cost, and monitoring.
Start with the 80%. Add the 20% only when the foundation is solid.
Major Takeaways
- Cognition is emergent from five biological systems. Optimize the systems (sleep, metabolism, autonomic regulation, mitochondria, hormones), and cognitive performance improves automatically. Trying to optimize cognition directly while systems are compromised is futile.
- Measurement enables optimization. Track HRV, sleep efficiency, blood biomarkers, cognitive performance. What gets measured gets managed. Use data to personalize—your biology determines what works.
- Recovery is adaptation. Stress without recovery is damage. Stress with adequate recovery is growth. The protocol engineers the stress-recovery cycle systematically.
- Consistency beats intensity. 80% adherence sustained long-term outperforms 100% adherence for 30 days followed by abandonment. Build sustainable practices, not heroic efforts.
- Individual response varies. Genetics, epigenetics, microbiome, stress load—all create individual variability. Personalize ruthlessly based on your data. Drop interventions that don't work for you.
- Biological optimization has costs. Hormetic stress, supplement tolerance, time investment, financial costs, risk of obsession. Optimize intelligently, not maximally. Respect your limits.
- This is infrastructure, not tactics. You're not learning productivity hacks—you're engineering the biological conditions where peak performance is possible. Build the infrastructure first, then optimize performance on top of it.
Now Execute.
The Bio-Performance Protocol isn't a quick fix. It's biological systems engineering requiring 60–90 days of disciplined implementation, ongoing measurement, and continuous personalization. The result: 20–40% cognitive enhancement sustained indefinitely.
Your brain is capable of extraordinary performance. The question is whether you'll provide the biological conditions it requires.
The protocols are here. The research is cited. The implementation guide is complete.
NOW EXECUTE“No man has the right to be an amateur in the matter of physical training.” — Socrates (via Xenophon)
What You Need to Remember
The ten biological truths that elite performers never ignore.
Hardware before software
No productivity system overrides bad sleep, poor fuel, or chronic sympathetic overdrive. Biology sets the floor — everything else builds on top of it.
Explore: Module 1 — The Biological Platform →Variables multiply, not add
Sleep × nutrition × movement interact multiplicatively. A 10% improvement in each produces a 33% compound gain — but a zero in any one collapses the entire equation.
Explore: Module 1 — Systems Integration →Your circadian clock outperforms every supplement
Working with your 24-hour rhythm — morning light, timed meals, evening wind-down — produces larger cognitive gains than any nootropic ever tested in clinical trials.
Explore: Module 2 — Circadian Architecture →Recovery debt is invisible until it isn't
You can't feel 12% cognitive decline from cumulative sleep restriction. You can't feel subclinical magnesium deficiency. By the time you notice, you've been operating impaired for months.
Explore: Module 3 — Recovery Debt →Your baseline shifts in 90 days
Neuroplasticity, hormonal adaptation, and metabolic flexibility are real. Your biological floor isn't permanent — it's the product of your last 90 days of behavior.
Explore: Module 3 — Adaptation Windows →More inputs, fragile outputs
Stacking supplements and stimulants on a broken recovery foundation creates performance that looks impressive and collapses under the first real stressor. Robustness beats peak.
Explore: Module 4 — Fragility Trap →Recovery separates the field
The gap between elite and average isn't training intensity — it's recovery quality. Sleep architecture, parasympathetic activation, and strategic deloading are the invisible advantages.
Explore: Module 4 — Recovery Science →Measure, then modify
Without baseline data on sleep, HRV, blood markers, and cognitive performance, optimization is guesswork with expensive supplements. Measurement turns speculation into engineering.
Explore: Module 5 — Self-Quantification →Protocols survive motivation failures
When motivation disappears — and it will — standardized routines for sleep onset, morning light, meal timing, and movement keep the biological machine running. Systems don't need willpower.
Explore: Module 5 — Protocol Design →Biology is a practice, not a project
There's no finish line. Your physiology changes with age, stress, seasons, and demands. The practice is perpetual calibration between protocols, data, and the body you have today.
Explore: Module 5 — The Ongoing Practice →Continue Your Journey
References
0 sources cited — journal articles and landmark studies in bioperformance optimization, metabolic switching, neuroplasticity, autonomic function, and cognitive enhancement
- 1(2017). The role of sleep in cognition and emotion. Annals of the New York Academy of Sciences, 1396(1), 32–51.
- 2(2013). Sleep drives metabolite clearance from the adult brain. Science, 342(6156), 373–377.
- 3(2011). Exposure to room light before bedtime suppresses melatonin onset and shortens melatonin duration in humans. Journal of Clinical Endocrinology & Metabolism, 96(3), E463–E472.
- 4(2014). Sleep and the price of plasticity: From synaptic and cellular homeostasis to memory consolidation and integration. Neuron, 81(1), 12–34.
- 5(1995). Contribution of the circadian pacemaker and the sleep homeostat to sleep propensity, sleep structure, electroencephalographic slow waves, and sleep spindle activity in humans. Journal of Neuroscience, 15(5), 3526–3538.
- 6(2011). Evening exposure to a light-emitting diodes (LED)-backlit computer screen affects circadian physiology and cognitive performance. Journal of Applied Physiology, 110(5), 1432–1438.
- 7(1999). Stability, precision, and near-24-hour period of the human circadian pacemaker. Science, 284(5423), 2177–2181.
- 8(2017). Sleep and human aging. Neuron, 94(1), 19–36.
- 9(2003). The cumulative cost of additional wakefulness: Dose-response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation. Sleep, 26(2), 117–126.
- 10(2013). Entrainment of the human circadian clock to the natural light-dark cycle. Current Biology, 23(16), 1554–1558.
- 11(2014). Impact of windows and daylight exposure on overall health and sleep quality of office workers. Journal of Clinical Sleep Medicine, 10(6), 603–611.
- 12(2012). Social jetlag and obesity. Current Biology, 22(10), 939–943.
- 13(2016). Can ketones help rescue brain fuel supply in later life? Implications for cognitive health during aging and the treatment of Alzheimer's disease. Frontiers in Molecular Neuroscience, 9, 53.
- 14(2018). Intermittent metabolic switching, neuroplasticity and brain health. Nature Reviews Neuroscience, 19(2), 63–80.
- 15(2008). Alzheimer's disease is type 3 diabetes—evidence reviewed. Journal of Diabetes Science and Technology, 2(6), 1101–1113.
- 16(2014). Fasting: Molecular mechanisms and clinical applications. Cell Metabolism, 19(2), 181–192.
- 17(2018). Flipping the metabolic switch: Understanding and applying the health benefits of fasting. Obesity, 26(2), 254–268.
- 18(2004). Effects of beta-hydroxybutyrate on cognition in memory-impaired adults. Neurobiology of Aging, 25(3), 311–314.
- 19(2012). The nervous system and metabolic dysregulation: Emerging evidence converges on ketogenic diet therapy. Frontiers in Neuroscience, 6, 33.
- 20(2017). β-Hydroxybutyrate: A signaling metabolite. Annual Review of Nutrition, 37, 51–76.
- 21(2006). Neuroprotective and disease-modifying effects of the ketogenic diet. Behavioural Pharmacology, 17(5-6), 431–439.
- 22(2013). Beyond weight loss: A review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets. European Journal of Clinical Nutrition, 67(8), 789–796.
- 23(2010). Beneficial effects of docosahexaenoic acid on cognition in age-related cognitive decline. Alzheimer's & Dementia, 6(6), 456–464.
- 24(2013). DHA supplementation improved both memory and reaction time in healthy young adults. American Journal of Clinical Nutrition, 97(5), 1134–1143.
- 25(2015). Long-chain omega-3 fatty acids and the brain: A review of the independent and shared effects of EPA, DPA and DHA. Frontiers in Aging Neuroscience, 7, 52.
- 26(2017). Omega-3 fatty acids and inflammatory processes: From molecules to man. Biochemical Society Transactions, 45(5), 1105–1115.
- 27(2014). Polyunsaturated fatty acids and their metabolites in brain function and disease. Nature Reviews Neuroscience, 15(12), 771–785.
- 28(2006). Role of omega-3 fatty acids in brain development and function: Potential implications for the pathogenesis and prevention of psychopathology. Prostaglandins, Leukotrienes and Essential Fatty Acids, 75(4-5), 329–349.
- 29(2014). Voluntary activation of the sympathetic nervous system and attenuation of the innate immune response in humans. Proceedings of the National Academy of Sciences, 111(20), 7379–7384.
- 30(2017). Heart rate variability and cardiac vagal tone in psychophysiological research. Frontiers in Psychology, 8, 213.
- 31(2009). Claude Bernard and the heart-brain connection: Further elaboration of a model of neurovisceral integration. Neuroscience & Biobehavioral Reviews, 33(2), 81–88.
- 32(2007). The polyvagal perspective. Biological Psychology, 74(2), 116–143.
- 33(2013). The promise of heart rate variability biofeedback: Evidence-based applications. Biofeedback, 41(3), 110–120.
- 34(2014). Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology, 5, 756.
- 35(2017). An overview of heart rate variability metrics and norms. Frontiers in Public Health, 5, 258.
- 36(2013). The relationship between mental and physical health: Insights from the study of heart rate variability. International Journal of Psychophysiology, 89(3), 288–296.
- 37(2023). Hallmarks of aging: An expanding universe. Cell, 186(2), 243–278.
- 38(2019). Maintenance of skeletal muscle mitochondria in health, exercise, and aging. Annual Review of Physiology, 81, 19–41.
- 39(2010). Mitochondria and neuroplasticity. ASN Neuro, 2(5), e00045.
- 40(2016). Mitochondrial biogenesis as a pharmacological target: A new approach to acute and chronic diseases. Annual Review of Pharmacology and Toxicology, 56, 229–249.
- 41(2013). Hallmarks of a new era in mitochondrial biochemistry. Genes & Development, 27(24), 2615–2627.
- 42(2008). Mitochondrial contributions to tissue damage in stroke. Neurochemistry International, 52(4-5), 638–645.
- 43(2018). Mitochondria and mitochondrial cascades in Alzheimer's disease. Journal of Alzheimer's Disease, 62(3), 1209–1227.
- 44(2007). Exercise builds brain health: Key roles of growth factor cascades and inflammation. Trends in Neurosciences, 30(9), 464–472.
- 45(2011). Exercise training increases size of hippocampus and improves memory. Proceedings of the National Academy of Sciences, 108(7), 3017–3022.
- 46(2013). Bridging animal and human models of exercise-induced brain plasticity. Trends in Cognitive Sciences, 17(10), 525–544.
- 47(2013). Exercise induces hippocampal BDNF through a PGC-1α/FNDC5 pathway. Cell Metabolism, 18(5), 649–659.
- 48(2016). Exercise promotes the expression of brain derived neurotrophic factor (BDNF) through the action of the ketone body β-hydroxybutyrate. eLife, 5, e15092.
- 49(2008). Be smart, exercise your heart: Exercise effects on brain and cognition. Nature Reviews Neuroscience, 9(1), 58–65.
- 50(2018). Effects of creatine supplementation on cognitive function of healthy individuals: A systematic review of randomized controlled trials. Experimental Gerontology, 108, 166–173.
- 51(2003). Oral creatine monohydrate supplementation improves brain performance: A double-blind, placebo-controlled, cross-over trial. Proceedings of the Royal Society B, 270(1529), 2147–2150.
- 52(2021). Creatine supplementation and brain health: A narrative review. Nutrients, 13(2), 586.
- 53(2011). The influence of creatine supplementation on the cognitive functioning of vegetarians and omnivores. British Journal of Nutrition, 105(7), 1100–1105.
- 54(2000). Human physiological responses to immersion into water of different temperatures. European Journal of Applied Physiology, 81(5), 436–442.
- 55(2010). What is the biochemical and physiological rationale for using cold-water immersion in sports recovery? A systematic review. British Journal of Sports Medicine, 44(3), 179–187.
- 56(2004). Winter swimming improves general well-being. International Journal of Circumpolar Health, 63(2), 140–144.
- 57(2016). The effect of cold showering on health and work: A randomized controlled trial. PLoS One, 11(9), e0161749.
- 58(2010). Is caffeine a cognitive enhancer? Journal of Alzheimer's Disease, 20(S1), S85-S94.
- 59(2008). The combined effects of L-theanine and caffeine on cognitive performance and mood. Nutritional Neuroscience, 11(4), 193–198.
- 60(2012). The cognitive-enhancing effects of Bacopa monnieri: A systematic review of randomized, controlled human clinical trials. Journal of Alternative and Complementary Medicine, 18(7), 647–652.
- 61(2010). Piracetam and piracetam-like drugs: From basic science to novel clinical applications to CNS disorders. Drugs, 70(3), 287–312.
- 62(2002). Design and study of piracetam-like nootropics: Controversial members of the problematic class of cognition-enhancing drugs. Current Pharmaceutical Design, 8(2), 125–138.
- 63(2006). Progress in studies of huperzine A, a natural cholinesterase inhibitor from Chinese herbal medicine. Acta Pharmacologica Sinica, 27(1), 1–26.
- 64(2003). Salvia officinalis extract in the treatment of patients with mild to moderate Alzheimer's disease. Journal of Clinical Pharmacy and Therapeutics, 28(1), 53–59.
- 65(2016). Establishing natural nootropics: Recent molecular enhancement influenced by natural nootropic. Evidence-Based Complementary and Alternative Medicine, 2016, 4391375.
- 66(2013). Gonadal steroids and body composition, strength, and sexual function in men. New England Journal of Medicine, 369(11), 1011–1022.
- 67(2005). Testosterone improves spatial memory in men with Alzheimer disease and mild cognitive impairment. Neurology, 64(12), 2063–2068.
- 68(2006). Testosterone and cognitive function: Current clinical evidence of a relationship. European Journal of Endocrinology, 155(6), 773–781.
- 69(2007). Neuropsychiatric aspects of hypothyroidism and treatment reversibility. Minerva Endocrinologica, 32(1), 49–65.
- 70(2014). Psychiatric and cognitive manifestations of hypothyroidism. Current Opinion in Endocrinology, Diabetes and Obesity, 21(5), 377–383.
- 71(2009). Effects of stress throughout the lifespan on the brain, behaviour and cognition. Nature Reviews Neuroscience, 10(6), 434–445.
- 72(1995). Stress and cognitive function. Current Opinion in Neurobiology, 5(2), 205–216.
- 73(2000). Glucocorticoids and hippocampal atrophy in neuropsychiatric disorders. Archives of General Psychiatry, 57(10), 925–935.
- 74(2016). B Vitamins and the brain: Mechanisms, dose and efficacy—A review. Nutrients, 8(2), 68.
- 75(2006). Effects of nutrients (in food) on the structure and function of the nervous system: Update on dietary requirements for brain. Part 1: Micronutrients. Journal of Nutrition, Health and Aging, 10(5), 377–385.
- 76(2009). Choline: An essential nutrient for public health. Nutrition Reviews, 67(11), 615–623.
- 77(2015). Magnesium in prevention and therapy. Nutrients, 7(9), 8199–8226.
- 78(2013). Low serum vitamin D concentrations in Alzheimer's disease: A systematic review and meta-analysis. Journal of Alzheimer's Disease, 33(3), 659–674.